 |
 |
Inomed ISIS
IOM
Starting from
August 2007, we are performing all pedicle
screw surgeries with the use of Inomed
special instrumentation for pedicular screw
monitoring. |
|
 |
| |
 |
Bulleted Lists
FP 2002 will sometimes
create your list within a table that does not
view as expected. Delete this table and insert
your own list. |
|
 |
| |
|
 |
 |
 |
 |
|
 |
| |
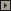 Surgical Standards:
Surgical Standards:
1. Skeletonization of L4, L5 laminae and the upper
border of the sacrum, performed, trying during that
, to check for movable segments, for further
intraoperative confirmation. It happened several
times, that the patient was planned for such a
procedure, and this trick , changed the plan of
surgery, before attempting to go far, to such areas
as the transverse processes. Using towel clips is a
useful tool for such task.
2. Check for recent fractures at the isthmus, since
malpractice of others especially in the third world,
by using a baton for LBP patients, which causing
fractures of the spinous process, lamina and
isthmus. To these special cases, which the patient
try to escape these events before surgery, I
modified a new technique by using miniscrews, after
drilling the surface of the bone , to accept three
or four screws from the orthopedic hand set screws.
It usually works excellent and the construct
becoming stable.
3. Remove the whole lamina of L5 with all the
cartilage, performing during that foraminotomy of
both S1 roots for not less than 10 mm distance.
Expose both L5 roots and remove all the compressing
elements. By doing this, you avoid any injury to
these roots , and nibbling with drilling down to the
pedicle, you actually not in need for fluoroscopy.
This also facilitate later the process of reduction.
Don't forget to gather the bone for subsequent
grafting.
4. Try all the time to preserve the epidural fat,
since it prevents subsequent fibrosis and in case,
of its poverty, you can transfer the most near local
fat tissue. These fatty tissues are more similar to
the epidural fat , than the subcutaneous or the fat
over the dorsal sheet, or other artificial
materials, with which I had in the past a bad
experience, such as the adcon-gel, which to my
knowledge is out of production.
5. Perform bilateral discectomy L5-S1, trying to
make the holes very small, to preserve the PLL and
the posterior aspect of the annulus fibrosis, to
prevent recurrent disc . Try meticulously clean the
disc space and try during that to reduce the
slippage by curved blunt metallic devices, they are
many. Observe the adjacent vertebral edges to notice
the difference in the level. Some times, you need to
perform tiny drilling at the level of the disc space
to insert the reducing device, as seen in the
present video.
6. Using the polyaxial transpedicular screws,
facilitate the easiness of rods placement and check
fluoroscopy must be done, in spite of the previously
mentioned exposed pedicles. Do not be confident, all
the time double check your actions. After inserting
the four screws, the rods must be a little bit
longer, to perform distraction and subsequent
reduction.
7. After your device in place and the reduction is
acceptable, and you are satisfied with the images,
check the roots and the pedicles, which could have
small cracks at the insertion canal and remove them,
to prevent any unnecessary malformed structures in
the roads. Check the disc space from both sides and
perform further discectomy, if needed.
8. The gathered bone, at the start of the operation
is chipped in small pieces and realigned lateral to
the rods with refreshment of the transverse
processes for future bony fusion. You must take in
consideration, that in some cases the construct
becoming loose and this graft can help in this
situation, in case of removing the device after
several months, so whatever the reason was.
9. During closure and fat tissue transfer, observe
the chips of bone so as to prevent them from
slipping to the neural elements. Water-tight closure
with subcuticular stitching, avoid Ready-vac drains.
10. Use
intraoperative monitoring with triggered myogenic
stimulation to avoid root irritation or damage
during the insertion of the pedicular screws.
|
|
 |
|
 |
|